Annual prostate cancer screening for men over 50, and even earlier for African American men and those with a family history of prostate cancer should be standard practice.
By Dr. Navin C. Shah*

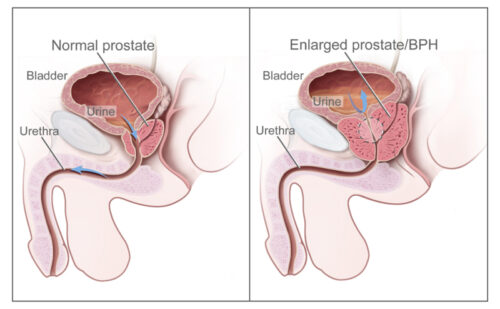
The prostate, a male gland located just below the bladder, is a critical component of the urinary system. As men age, particularly those over 50, the prostate often enlarges, leading to symptoms like urinary hesitancy, incomplete bladder emptying, slow urinary stream, and frequent nighttime urination. Moreover, prostate cancer, more prevalent in African American men and those with a family history of prostate cancer, becomes a concern in this demographic.
Early detection of prostate cancer is crucial, as the disease is generally curable in its initial stages through various treatment modalities such as surgery, radiation, or drugs. Unfortunately, once the cancer has metastasized, achieving a cure becomes exceedingly difficult, and the prognosis turns grim.
Since the implementation of prostate cancer screening guidelines by the U.S. Preventative Services Task Force (USPSTF) in 2012, an unsettling trend has emerged: a surge in reported cases, increased metastasis, and a higher mortality rate, particularly in men aged 65 and older. A study examining 26,168 patients with metastatic cancer revealed that a staggering 78 percent succumbed to prostate cancer, with 59 percent facing mortality within the first two years.
Treating metastatic prostate cancer is not only challenging but also financially burdensome, with each injection costing a substantial $40,000, offering only a marginal extension of life.
Annual prostate cancer screening, involving a digital rectal examination (DRE) and a blood test measuring Prostate Specific Antigen (PSA), is a cost-effective method for early detection. The blood test, priced at $25, serves as an accessible diagnostic tool. Abnormalities in either the DRE or PSA, or both, prompt a prostate biopsy, offering insights into the presence and grade of prostate cancer.
READ: Men less aware about sexual health risk post prostate surgery (January 11, 2016)
Despite the imperfections in current prostate cancer screening guidelines, the disease remains the most common cancer in men and the second leading cause of cancer-related deaths in the United States. In 2021, the American Cancer Society reported 248,530 new prostate cancer cases and 34,130 prostate cancer-related deaths. African American men and those with a family history of prostate cancer face a higher incidence of the disease and increased rates of metastasis.
The American Cancer Society recorded a concerning trend in the last five years (2017-2022), with 107,103 new prostate cancer cases and 7,700 additional deaths due to prostate cancer. The impact of decreased prostate cancer screening is evident, emphasizing the urgent need for proactive measures.
For cases of low-grade cancer, active surveillance (AS) is recommended, supported by a follow-up prostate biopsy. However, recent research highlights the limitations of this approach, revealing higher-grade prostate cancer in subsequent biopsies for 60 percent of African American and 48 percent of white patients under active observation.
I propose that annual prostate cancer screening for men over 50, and even earlier for African American men and those with a family history of prostate cancer, becomes standard practice. Leveraging advancements such as MRI biopsies, active surveillance, genetic testing, and PSMA PET/CT scans for metastasis can significantly decrease prostate cancer morbidity, mortality, and cost of treating prostate cancer. It is time to prioritize early detection, offering the best chance for a cure and improved quality of life for men at risk of prostate cancer.
(Dr. Navin C. Shah is a urologist based in the Washington, D.C., area. He has published six papers on prostate cancer and 15 letters to the editor commenting on other published papers on prostate cancer in various reputed US urology journals. His memoir, “Karma and Destiny of an Indian American Surgeon” (published by AB Books), was released last year. Dr. Shah is also a numismatist with a collection of thousands of ancient Indian coins.)